Category: Uncategorized
SCWIHERC’s Current Solicitation Opportunities
View current postings for doing business with SCWIHERC!
November 9, 2022 Membership Meeting
SCWIHERC 11-9-22 Meeting Notes
Recording: https://us06web.zoom.us/rec/share/PQWEweQMuvett1Y6doMZ2uxAiWsRWIxKJ2e-ShmfTi13VDo0zbQRmaUqARLRCylN.FFBdmVxW9rubyYJ7
Passcode: See email sent November 10
Hospital Meeting:
EMResource reminders- PEDs surge bed count, update at least once daily, not going away as long as surge is an issue. PEDS ED Boarders expected to go up
ABLS- next batch expiring in February, sending periodic updates. Seat allocation: 5 nonphysician seats for each level III, IV and unclassified, 12 nonphysician setas for each level I and II. 2 physician seats for each hospital. Reach out at any time to enroll new students, check assignment, with other questions.
Open discussion: violent patients and patient security screening. Barriers to implementation- staffing. Seeing increase in threats from patients/visitors. Not necessarily weapons, but more physical aggression/assault directed at staff. Is incidence increasing, or reporting increasing? Both. Increasing visitors d/t decreasing COVID restrictions is a factor.
De-escalation options: Crisis Prevention Institute Nonviolent Crisis Intervention, MOAB (management of aggressive behavior), increasing posted signage on patient/visitor behavior expectations, higher security presence in facility, DT4EMS, active threat drills at service level. Safety solution in another state: installed hotel safes in trauma bays to store contraband/weapons while the patient was admitted, have security staff move weapon off patient. Some states have quite intensive security screening procedures compared to us. Shared escalation policy- green, yellow, red, full lockdown, policy shared by email November 10.
HCID discussion: need a review of Ebola state ConOps and how ETCs/Regional Treatment Centers are involved, include transportation plan.
Membership Meeting:
Leadership review SCWIHERC and OPEHC: http://www.scwiherc.org/category/who-are-we/ or first tab of Coalition phone book in SCWIHERC shared drive.
Fiscal and Sustainability Update- The HERCs have been presented with a lot of new policies that impact how we do business. Grant funds are only reimbursable after expenses have been incurred, so how do we solve cash flow to pay for vendors and services up front? Historically have had the benefit of having a fiscal agent, but now that we are an incorporated legal entity, this is not allowed anymore. Current coping mechanism is HERC staff have been putting expenses on personal credit, which is not advisable or sustainable. To better explore options, SCWIHERC will be recruiting a Sustainability Coordinator to explore our options for revenue sources and cash flow issues. Sustainability Coordinator Request for Application emailed and posted to scwiherc.org on November 10. SCWIHERC Board welcomes any and all suggestions and ideas on how to cope with these issues. Additional fiscal policies that have been recently updated include a Net 30 days from submission turnaround time on funding disbursement, we cannot spend grant funds on food, any HERC travel is reimbursed at the state rate (previously was federal rate), must use state procurement guidelines for competitive bids, and all HERC expenses must be explicitly approved by the state ahead of time to be reimbursed.
Training, Exercises, SALT Triage and RMCC Project and Training: Training needs assessment was sent out October 26, sent again November 10, due Nov 30. Your input is requested and valued!
Working on request for application to find a contractor to assist with planning and conducting our Medical Response Surge Exercise (MRSE), which replaced the Coalition Surge Test (CST) from the before COVID times. This exercise will also test our pediatric surge plan to satisfy another grant deliverable. Plan to use a Wisconsin Dells peak tourism season scenario for surge. Other planned TTX is for radiological surge, which is the topic of our specialty surge annex this year.
Still continuing with SALT Triage and Regional Medical Coordination Center project and training. Offered 5 first receiver train the trainer sessions in May, about half of hospitals participated. Still hoping to have other hospitals participate, please reach out to plan a regional training or to request triage ribbon kits or replacement ribbons. Youtube training video for hospitals: https://www.youtube.com/watch?v=N7OG8a7vXnE
Also continuing to offer similar training to EMS agencies in the region, also incorporating training on RMCC resource-activation and coordination. Reach out to schedule these sessions!
Will Koehne, WI DHS OPEHC Epidemiologist, gave an interview of Hospital Dashboards on PCA Portal, review recording, email Jennifer or Will William.koehne@dhs.wisconsin.gov for access. Other systems’ discussion deferred at this time.
RSV surge- Please update bed count (green banner) daily! What will be the issues with PEDs surge? Short on pediatric providers and staff for both ED and inpatient. Some have developed some education for nursing and family practice to augment clinical care- partner with your respiratory therapy! Jennifer will forward clinical resources from the National Pediatric Disaster Coalition/AAP to hospitals.
No reports of diesel fuel shortage in the region at this time, but have seen elsewhere in the state. Be sure you have a priority contract with your vendor and please relay any news of shortages to Jennifer and your county emergency manager for situational awareness.
No reports of albuterol shortage in the region at this time, but have seen elsewhere in the state. Reports of etomidate, fentanyl, and racemic EPI shortages.
Doug Hill gave an update on Crisis Standards of Care. Note that Wisconsin Hospital Mutual Aid MOU will be sunsetting and not renewed, due to a lack of interest from hospital leaders and WHA. Refer to recording and this 2010 WHA document he referenced: https://www.wha.org/WisconsinHospitalAssociation/media/WHACommon/EmergencyPrep/HospitalsGuideforMassCasualtyEvents6-2010.pdf
Doug Hill can be reached at djh1967@gmail.com
Meeting attendance:
Matt Bartol- Dodge County HHS, EM
Tom Ellison- UW Health
Lyle Kratochwill- Richland Hospital
Christal Foreyt- Gundersen Boscobel
Mary Crowley- Juneau Co HD
Amanda Diedrich- Juneau Co HD
Sarah Jensen- Marquette Co HD
Jodi Moyer- Beloit Health System
S Eaton
Donna Haugom- Jefferson Co EM
Tina Strandlie- Stoughton
Belle Koch, Sauk Prairie Hospital
Carmen Luther- Reedsburg Area Med Ctr
Jim Abitz- Southwest Health
Ron Krause- Mercyhealth
Matt Christian- Marshfield Med Ctr Beaver Dam
Jennylynde Packham- UW Health Rehab
Dan Williams- SCRTAC
Adrianne Bonow
Eric Anderson- Dane County EM
Dave Larson- Madison VA
Mike Stephens- UW Health
Steve Haskell- UW Health
Nathan Bubenzer- Meriter UPH
Katie Budack- Grant Regional
Dave Kitkowski- St. Clare Baraboo
Sam LaMuro- Fort HealthCare
Jodie Molitor- Sauk Co HD
Nina Gregerson- PH Madison and Dane County
Leanne Siefert- Watertown Regional Med Ctr
Karen Greenwald- Dodge Co HD
Kimberley Spurgeon- Family Health La Clinica
Heather Poker- St. Mary’s Madison
Tammy Kingery- Gundersen Moundview
Samroz Jakvani- Jefferson Co HD
Laura Kane- UW Health
Sally Blackbourn- Memorial Hospital of Lafayette Co
Carrie Meier- Dane Co EM
Sharone Rateike- St. Mary’s Janesville
Elizabeth Chilsen- Jefferson Co HD
Nick Metz- Upland Hills Health
Victoria Parker- Watertown HD
Lynn Skatrud- Green Co HD
Emily Kosterman- Waupun Memorial
Jane Gervais- Adams Co EM
Jeff Kindrai- Grant Co HD
Colton Ritchie- PH Madison and Dane County
Ken Van Horn- PH Madison and Dane County
Tanna McKeon- Green Co EM
Debbie Siegenthaler- Iowa Co HD
Andrea Murleau
Madison Dillinger
Chad Atkinson- Mercyhealth Janesville
Will Koehne- WI DHS OPEHC
Doug Hill- CSC Project
Aurielle Smith- PHMDC and SCWIHERC
Mike Lohmeier- UW Health and SCWIHERC
Jennifer Behnke- SCWIHERC
SCWIHERC Network Recovery Exercise April 12
Our Network Recovery Exercise took place on April 12, thank you for your participation. The After Action Report and Improvement Plan will be shared when it is available.
SCWIHERC Hospitals See High Patient Volumes, Limited Resources – News Release
FOR IMMEDIATE RELEASE
September 10, 2021
Hospitals in South Central Wisconsin see high patient volumes, limited resources
Hospitals seek community help to prevent COVID-19 cases putting critical strain on regional healthcare systems
Hospitals and healthcare facilities throughout southcentral Wisconsin are experiencing a high volume of inpatients, limiting hospital beds and putting a strain on resources.
This serious situation is occurring across the 14 counties of the South Central Wisconsin Healthcare Emergency Readiness Coalition, (SCWIHERC). Its member hospitals are asking for our communities’ help.
To better control the situation, the hospitals are urging everyone to continue being vigilant with COVID-19 safety measures, such as receiving any COVID-19 vaccine, masking, and physically distancing where appropriate.
This present high volume of patients spans across critical care areas of the hospitals, like intensive care units (ICU), general medical floors, and emergency departments. With resources stretched, it is becoming more difficult to receive care close to home if you may need it for COVID and non-COVID-related illnesses.
From July 28 to Sept. 1, the total number of COVID-19 hospitalizations increased four-fold in the South Central region. In that same timeframe, there were 5.5 times the number COVID-19 ICU hospitalizations. Many rural hospitals have no or limited ICU capability and are all reliant on the same limited ICU beds in larger cities, including Madison.
While the current high volume in healthcare facilities in the region is a mixture of COVID-19 and non-COVID-19 patients, a rise in preventable COVID-19 admissions is a driving factor. Preventing a further rise in COVID-19 admissions is our focus in this critical time.
In fact, COVID-19 infections requiring hospitalization are increasing at a similar rate to last winter’s surge. With students from pre-K through college returning to classrooms, the Labor Day holiday, and colder weather soon driving people indoors, additional increases are expected which could stretch resources to critical levels.
To receive a COVID-19 vaccine, please contact your local healthcare providers, or visit the state Department of Health Services vaccine webpage.
###
The South Central Wisconsin Healthcare Emergency Readiness Coalition (SCWIHERC) is a coalition that collaborates with 29 area hospitals and numerous other healthcare providers over 14 counties to prepare for and respond to emergencies in South Central Wisconsin.
SCWIHERC Members signing this message:
| Organization | Media Contact Name and Email (if provided) |
| South Central Wisconsin Healthcare Emergency Readiness Coalition | Jennifer Behnke (jennifer.behnke@scwiherc.org) |
| Aspirus Divine Savior Hospital and Clinics | Haley Gilman (haley.gilman@aspirus.org) |
| Beloit Health System | Megan Goggin (mgoggin@beloithealthsystem.org) |
| Edgerton Hospital and Health Services | |
| Grant Regional Health Center | |
| Gundersen Health System | Chris Stauffer (cjstauff@gundersenhealth.org) |
| Marshfield Medical Center – Beaver Dam | Dan Baulch (baulch.dan@marshfieldclinic.org) |
| Memorial Hospital of Lafayette County and Primary Care Clinics | |
| Mercyhealth | Rebecca Rose (rrose@mhemail.org) |
| Mile Bluff Medical Center, Mauston | |
| Prairie Ridge Health | |
| Reedsburg Area Medical Center | Robert Van Meeteren (rvanmeeteren@ramchealth.org) |
| The Richland Hospital | Lyle Kratochwill (lyle.kratochwill@richlandhospital.com) |
| Sauk Prairie Healthcare | Amy Ryan (amy.ryan@saukprairiehealthcare.org) |
| SSM Health | Lisa Adams (Lisa.Adams@ssmhealth.com) |
| Southwest Health | Jaime Collins (collinsj@southwesthealth.org) |
| Stoughton Health | Laura Mays (lmays@stoughtonhealth.com) |
| UnityPoint Health – Meriter | Nicole Aimone (Nicole.Aimone@unitypoint.org) |
| UW Health | Andrew Hellpap (AHellpap@uwhealth.org) |
| Watertown Regional Medical Center | Steve Hunt (Steven.Hunt@watertownregional.com) |
| William S. Middleton Memorial Veterans Hospital | Paul Rickert (paul.rickert@va.gov) |
COVID-19 After Action Review
SCWIHERC will be hosting a COVID-19 After Action Review on September 22.
November 4, 2020 Meeting
SCWIHERC General Membership Meeting November 4, 2020 Notes
Meeting recording (expires May 4, 2021): https://transcripts.gotomeeting.com/#/s/d6b15298f36934f6312486e2957d822d8628f6199003b08f25da175c27eea927
Doug Hill gave an update on COVID-19 Crisis Standards of Care, including the work being done by the State Disaster Medical Advisory Committee (SDMAC). The state is expected to release guidance that mimic’s that of the National Academy of Medicine for COVID-19 vaccination priority groups. Refer to the following documents:
Framework for Equitable Allocation of COVID-19 Vaccine from the National Academy of Medicine:
https://www.nap.edu/read/25917/chapter/1
This figure is on page 30 of the PDF. Wisconsin’s guidance is likely to mirror this approach:
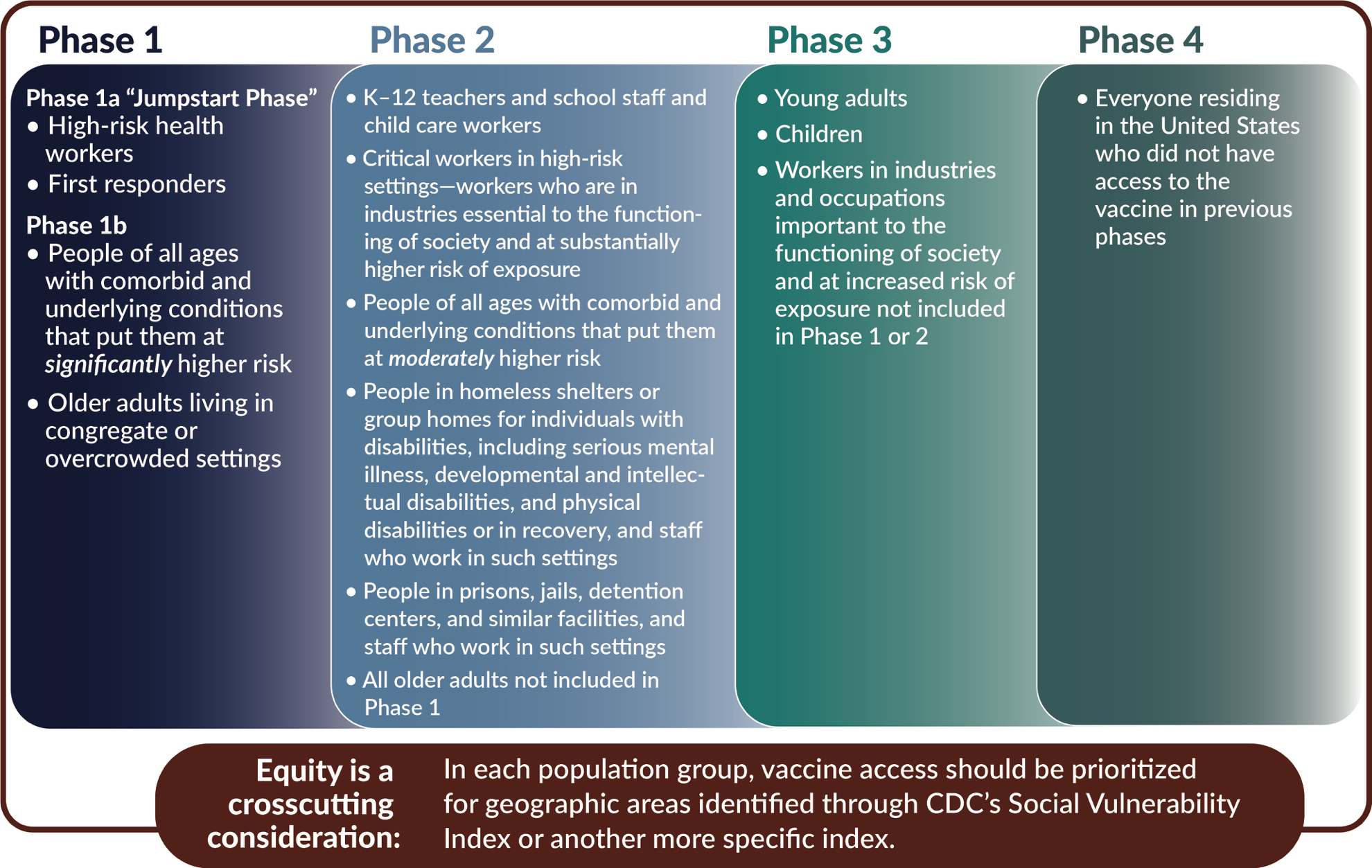
(Share Ethical standards document here)
Kevin Wernet gave an update on Mortuary Affairs and mass fatality planning. Key points:
Reach out early to your local EM if you have needs (body bags, cold trailers)
Observe practices that respect the decedent.
Move decedents out of their unit bed. If there is no room in your morgue, consider meeting the funeral home director at an entrance rather than bringing them into your facility and onto the patient care units. Leaving the decedent on the unit and having the funeral home pick up from the unit directly increases their exposure and PPE burn rate.
Kevin also gave an update from the PPE task force.
Key message: every N95 mask that is discarded instead of decontaminated is one less mask we have during this pandemic and for flu season. If internal resources are not available for decon, everyone is eligible to use the Battelle System.
See Respirator Reuse Guidance: https://www.dhs.wisconsin.gov/publications/p02699.pdf
Email Kevin with any questions on these topics: kevin.wernet@wisconsin.gov
Updates
Hospitals- please fill out the Match survey to capture hospital involvement in real events and exercises. It takes about 10-15 minutes if you have your AAR handy. We use this information to capture your in-kind efforts to meet our required 10% match of our federal grant. Link: https://www.surveygizmo.com/s3/3321278/WHEPP-Exercise-and-Real-Event-Report-F-02007-01-2017
SCWIHERC COVID-19 Mass Vaccination Functional Exercise is rescheduled for December 9, deadline to register is November 25. To be determined if we will have a spring exercise. Healthcare Recovery TTX that was originally scheduled for spring 2020 may be postponed to fall 2021 depending on vaccination efforts.
We are offering a virtual condensed public information officer 4 hour course soon. This course does not replace the G290 PIO curriculum (a 16 hour course), but offers a training for partners in PIO roles that have not been able to take formal training. The goal is to balance current demands due to COVID surge with the need to deliver this course in time to use the skills learned when communicating with the public regarding COVID-19 vaccination efforts. We conducted a poll during the meeting to determine when to schedule the course. Update: January was the top choice, we are looking at scheduling in early-mid January.
There are also many virtual training offerings available to keep up on your skills and knowledge since we cannot offer in-person trainings at this time. Refer to
Center for Domestic Preparedness Virtual Instructor-Led Training: https://cdp.dhs.gov/vilt
Wisconsin Emergency Management virtual offerings (in purple): https://www.trainingwisconsin.org/Schedule.aspx
The list produced by Svea Erlandson and Mariel Torres, our WI DHS Training and Exercise Coordinator and Specialist.
HERC Virtual Training Resources
We resumed our weekly SCWIHERC COVID-19 discussion and gave organizational updates.
Meeting attendance:
Brad Armstrong, UPH Meriter
Diana Quinn, SSM Health
Jodi Moyer, Beloit Health Systems
Nathan Bubenzer, UPH Meriter
Sharon Warden, Mile Bluff Medical Center
Alice Salli, Mendota Mental Health Institute
Alison Chouinard, Rock Co Health Dept
Angie Cohen, Grant Regional Health Ctr
Ben Eithun, UW Health/AFCH/SCWIHERC
Bill Ritzer, Reedsburg Area Medical Center
Brian Allen, Southwest Health
Carrie Meier, Dane County EM/EMS
Dave Larson, Madison VA
Deanna Wright, Memorial Hospital of Lafayette Co
Debbie Siegenthaler, Iowa County Health Dept
Diana Arneson, Rock County
Donna Haugom, Jefferson County EM
Gail Scott, Jefferson Co Health Dept
Steve Haskell, UW Health
Jane Gervais, Adams Co EM
Jodie Molitor, Sauk Co Health Dept
Jon Erdmann, Divine Savior
Josh Kowalke, Reedsburg Area Ambulance
Julie Leibfried, Lafayette Co Health Dept
Kacey Kronenfeld, Madison Emergency Physicians
Kate Stauffacher, Recover Health
Ken Kaiser, Grant Regional Health Ctr
Brenda Koehler-Borchardt, Watertown Regional Medical Ctr
Kristin Osterday
Laura Kane, UW Health
Leslie Cody, Allay Home and Hospice
Lisa Herritz, Ho Chunk Nation Health Dept
Patrick Monckton, Southwest Health
John Pettey, St. Mary’s Madison
Bob Swenarski, St. Mary’s Janesville
Sally Blackbourn, Memorial Hospital of Lafayette Co
Sam LaMuro, Fort Health Care
Sharon Foley, Divine Savior
Stephanie Novak, Marquette Co Health Dept
Tina Strandlie, Stoughton Hospital
Anna Taylor, Monroe Clinic
Carmen Luther, Reedsburg Area Medical Center
Lyle Kratochwill, Richland Hospital
Ashley Vickers, Mercy Walworth
Mary Crowley, Juneau County Health Dept
Guests: Doug Hill, WI DHS Crisis Standards of Care; Kevin Wernet, Wisconsin Emergency Management
Facilitated by Jennifer Behnke
Request for Proposal: Points of Dispensing Functional Exercise and COVID-19 After Action Review
SCWIHERC is seeking proposals for two separate events: a points of dispensing functional exercise and a COVID-19 After Action Review.
If you are interested in submitting an RFP, please see the attached documents and submit proposals electronically to Jennifer Behnke by close of business, July 8, 2020. Entities wishing to be considered for both exercises should submit separate proposals for each exercise.
Points of Dispensing RFP:
POD FE RFP
COVID-19 After Action Review RFP:
COVID-19 AAR RFP
March 5, 2020 Meeting
Join us for our March 5 meeting, see the agenda for details:
Recording available until September 6, 2020: https://transcripts.gotomeeting.com/#/s/67b8068bf4188a54d212fee56709134c0d2a1faef818fe85a53ef4ed29a0922a
Reminders:
See separate trainings list for upcoming trainings.
Please monitor WISCOM HRCRD5 open/clr at all times. WISCOM should be used to verbalize EMResource/WI Trac alerts for redundancy.
Please remember to submit the MATCH survey for all hospital-based exercises and real events using this link:
We had an in-depth discussion about COVID-19 Preparedness and Response. WI DHS created a survey to assess the PPE situation for all partners in the state, and this survey data is being shared with federal partners to assess the need to mobilize stockpiles, so please fill out the survey emailed out by Jennifer. Please find the one best representative in your facility to respond to the survey to avoid conflicting duplicate survey responses. Feel free to fill out the survey multiple times if the PPE situation in your organization changes. The SCWIHERC COVID-19 briefings will continue weekly until further notice.
The next portion of the meeting was dedicated to the Coalition Surge Test After Action Review and Facilitated Discussion. This information can be found in the after action report when available.
The Hospital and Medical Surge workgroups met in the afternoon and discussed surge planning in response to respiratory virus season and COVID-19, as well as MCI readiness. Three resources were shared by Jennifer:
CDC Mass Casualty Predictor Model
https://hsdl.org/?view&did=24463
Trauma centers: Prepare for mass casualty incidents by understanding the 10 predictable stages of disruption
Strategies for Improved Hospital Response to Mass Casualty Incidents
Meeting attendance:
Ashley Buys- UW Health
Jacob Greenberg- UW Health
Mary Crowley- Juneau Co HD
Lisa Herritz- Ho Chunk Nation HD
Laura Kane- UW Health AFCH
Asa Rowan, Community Health Systems
Sheryl Krause- Fort Healthcare
Brenda Koehler-Borchardt- Watertown Regional Medical Ctr
Jeff Kindrai- Grant County HD
Thomas Ellison- UW Health
Joe Meagher- Dodge Co EM
Amy Nehls- Dodge Co EM
Dave Larson0 Madison VA Hospital
Jane Gervais- Adams Co EM
Samantha Marcelain- Gundersen Moundview
Christal Foreyt- Gundersen Boscobel
Joni Marty- Green Co HD
Alison Chouinard- Rock Co HD
DeAnn McAllan- American Red Cross
Mary Tesserdorf- Monroe Clinic
Jodi Moyer- Beloit Health System
Johnny Holt- St. Clare Baraboo
Jon Erdmann- Divine Savior
Sharon Foley- Divine Savior
John Rago- Baraboo EMS
Julie Gorman- Sauk Prairie Healthcare
Abigail Kuehn- Watertown HD
Victoria Parker- Watertown HD
LuAnn Reuter- Prairie Ridge Health
Karen Sell- Prairie Ridge Health
Kyle Schaefer- UW Health
Jeff Ethington- UW Health OPO
Julie Muhle- Marshfield Medical Center Beaver Dam
John Pettey- St. Mary’s Madison
Jennifer Behnke- SCWIHERC
Online:
Dave Kitkowski- St. Clare Baraboo
Tana Buss- UW Health
Emily Kosterman- Waupun Memorial
Sue Matye- Iowa Co HD
Tanna McKeon- Green Co EM
Stephanie Kuschel- MercyHealth Janesville/NIPARC
Jen Boigenzahn- Gundersen
Carol Brown- Rainbow Hospice
Sarah Hughes- PH Madison Dane Co
Kathy Noe-
Sharon Rateike- St. Mary’s Janesville
Patrick Monckton- Southwest Health
Brian Allen- Southwest Health
Erin Hastert- Lafayette Co HD
Angie Cohen- Grant Regional Health Center
November 20, 2019 Meeting
November 20, 2019 Membership Meeting Notes
SCWIHERC Updates:
As of October 23, SCWIHERC is incorporated, now we are seeking nonprofit status to help support our long-term sustainability.
Our spring tabletop exercise topic is healthcare system recovery. The scenario will be written to engage all core partners: hospitals, public health, EMS, emergency management, and other healthcare providers. Tentative dates are April 14-16. We need exercise design team members, please let Jennifer know if you are interested in being on the design team.
The coalition surge test will be taking place again in late winter. We need to simulate evacuation of 430 patients to meet our 20% surge threshold required by our grant. If you are interested in volunteering to be an evacuating hospital, please let Jennifer know. If we do not have enough volunteers, we will ask hospitals directly to meet our federal requirements.
A training matrix was distributed listing all upcoming trainings for the remainder of the grant year. That information is summarized here: http://www.scwiherc.org/category/training/http://www.scwiherc.org/category/training/
CORRECTION: the training matrix had an error, the PER 211: Medical Management of CBRNE Incidents is May 18-19, NOT May 17.
Tracey Froiland, Fox Valley HERC Coordinator, presented on their Infectious Disease Go-Team. They pioneered this novel concept of forming a team to care for high consequence infectious disease patients in their home using telemedicine. This specially-trained team can also support caring for these patients in a hospital setting. See their promotional video for more info: https://www.youtube.com/watch?v=L4O3ZWkJgJ8
Tracey’s slides will be available in the SCWIHERC shared drive soon.
We had several partners present on different organizations that provide human personnel assets used in response. Presentation highlights:
WEAVR- Wisconsin Emergency Assistance Volunteer Registry: https://weavrwi.org/
Individual registry- Wisconsin’s ESAR-VHP. A database of individuals who can support the health needs of an incident. Pre-registered individuals have been vetted through a background check and credential verification. Individuals who are registered in WEAVR and deployed through a WEAVR request during a federal or state declared emergency are offered liability protection through Wisconsin Statute 257. The state is seeking clarification from the Office of Legal Counsel on whether this liability protection is available in the absence of federal or state declaration.
Registration in WEAVR is not a commitment to serve in any emergency. Please encourage your staff and partners to register!
MRC- Medical Reserve Corps. Brenda Lutz-Hanson presented on the Region 4 MRC and the purpose, mission, and sustaining of MRCs in Wisconsin. The entry point for MRCs in Wisconsin is registering in WEAVR and selecting the affiliation with an MRC. Currently, Region 5 (SCWIHERC’s region) has no active MRCs. Managing an MRC is often, but not always, done by local health departments. There is some work involved, but federal grant dollars may be available to support this effort. Contact Jennifer for more information.
DMAT- Wisconsin’s Disaster Medical Assistance Team. Patty Scanlin presented on this asset. They deploy outside of Wisconsin to assist medical operations after disasters and for large, planned events such as presidential funerals or inaugurations. They have field hospital capabilities. DMAT personnel are vetted by the federal process that takes 1-2 years and train on personal time, but are paid during deployment. Deployment notice may be as short as 12-24 hours, and deployments can last from 10-14 days.
American Red Cross- Connie Miley spoke about the volunteer capabilities and opportunities with American Red Cross. They often support sheltering and mass care operations all over the state and country.
Team Rubicon- Jodi Moyer spoke the mission and capabilities of Team Rubicon. They deploy nationally and focus on debris cleanup but have other capabilities. They are a veteran founded organization and 75% of their volunteer force is veterans. They are supported by donations from individuals and companies, and receive no payments by individuals impacted by disasters.
A question came up about requesting and utilizing any of these resources. It is strongly recommended that all requests are made through local emergency management. This helps ensure that those affected receive the most appropriate resource for their needs, and also may have reimbursement ramifications if federal or state funding is available for incident response and/or recovery.
Svea Erlandson, WI DHS Training and Exercise Coordinator, facilitated our Training and Exercise Planning Workshop in the afternoon. We reviewed data from the training needs assessment survey, and then had a productive conversation about developing training priorities and how to support these with available trainings. The three training priorities identified included Ensuring the Continuity of Healthcare Service Delivery, Catastrophic Event Preparedness for the Health Sector, and Health Emergency Management Orientation for partners in Wisconsin. These priorities will guide trainings offered in the July 1, 2020 to June 30, 2021 grant year.
Our meeting concluded with discussion on special populations and triaging the most important needs according to life safety priorities.
Grant guidance on this topic: Support HCC members with situational awareness and information technology (IT) tools already in use that can help identify children, seniors, pregnant women, people with disabilities, and others with unique needs. Support HCC member agencies in developing or augmenting existing response plans for these populations, including mechanisms for family reunification. Identify potential health care delivery system support for these populations (pre- and post-event) that can prevent stress on hospitals during a medical surge event. Assess needs and contribute to medical planning that may enable individuals to remain in their residences during certain emergencies. When that is not possible, coordinate with the jurisdiction’s ESF-8 lead agency to support the jurisdiction’s ESF-6 (Mass Care, Emergency Assistance, Housing, and Human Services) lead agency with access to medical care including at shelter sites. Coordinate with the jurisdiction’s ESF-8 lead agency to assess medical transport needs for these populations.
Jennifer also offered a definition for those with access and functional needs according to FEMA: Children and adults with physical, mobility, sensory, intellectual, developmental, cognitive, or mental health disabilities. Older adults. People with temporary or chronic health conditions (including taking daily medication). Women in late stages of pregnancy. People needing bariatric equipment. People with limited English proficiency, low literacy, or additional communications needs. People with very low incomes. People without access to transportation. People experiencing homelessness.
Based on this guidance and definition, the group identified these most urgent life safety priorities:
Electricity dependent individuals- how to find them before the incident, how to empower them to prepare for a power outage, how to care for them during a power outage, and how to partner with other groups to support these three capabilities. This includes home health, durable medical equipment suppliers, primary care providers.
Individuals with unreliable transportation options- planning for those who need transportation assistance for their medical appointments, and for those who don’t have the transportation means to evacuate when a community evacuation is ordered.
Individuals on medications for medical conditions- helping these individuals maintain an adequate supply of medications before an incident so they don’t run during an incident when normal suppliers may be disrupted, or if they cannot travel to refill meds. This includes working with other healthcare providers to share this message with vulnerable patients.
Supporting Home Health Agency Continuity of Operations- recognizing that HHAs are critical to keeping individuals with various conditions healthy and able to live at home, we will look for ways to support HHA continuity of operations so they can continue to do what they do every day even after a large or disruptive incident.
Meals on Wheels- supporting these agencies that meet the basic dietary needs of vulnerable individuals on a daily basis so that they can continue this important mission even after incidents.
Supporting better communications for these special populations, including the English as a second language community and those with low literacy levels. Not only translating written materials and having sufficient interpreter services available for every step of preparedness, response, and recovery, but also utilizing multiple channels of information dissemination. This can include traditional media channels like television, radio, and print, but also cultural and faith-based organizations that serve a role in gathering and outreach to these individuals and groups.
Important partners to engage in supporting these important missions can include local human services agencies, primary care organizations, home health agencies, long-term care organizations, Aging and Disability Resource Centers, WIC (Women, Infants, and Children) nutrition programs, 211 and United Way, and cultural and faith-based organizations.
The next steps proposed by the group include inviting representatives from these important partners to a round-table discussion to more thoroughly explore how we can work with these partners to promote preparedness, and support response and recovery efforts for these special populations.
Meeting Attendance:
Bob Swenarski- St. Mary’s Janesville
Juan Cullum- Mercyhealth Janesville
Jodie Molitor- Sauk County Health Dept
Alice Salli- Mendota Mental Health
Mary Crowley- Juneau County Health Dept
Lisa Herritz- Ho-Chunk Nation Health Dept
Asa Rowan- Community Health Systems Beloit
Gail Scott- Jefferson County Health Dept
Samantha LaMuro- Fort Healthcare
Mike Hall- Monroe Clinic
Kelly Pederson- St. Mary’s Madison
Nikki Salas- Watertown Regional Med Ctr
Brenda Koehler Borchardt- Watertown Regional Med Ctr
Marie-Noel Sandoval- Rock County Health Dept
Douglas MacFarlane- Crossroads Care Center of Mayville
Tina Strandlie- Stoughton Hospital
Christal Foreyt- Gundersen Boscobel Hospital and Clinics
Josh Kowalke- Reedsburg Ambulance
Jill Lenz- Columbia County Health Dept
Susan Lorenz- Columbia County Health Dept
Mike Lohmeier- SCWIHERC Medical Advisor
Carrie Meier- Dane County Emergency Mgmt
Connie Miley- American Red Cross
Jon Erdmann- Divine Savior Healthcare
John Longo- WI DHS OPEHC
Tracey Froiland- FVHERC
Mike Stephens- UW Health
Sarah Mattes- Public Health Madison Dane County
Steve Haskell- UW Health
Patricia Scanlin- UW Health TAC, WI DMAT
Sharon Foley- Divine Savior Healthcare
Alison Chouinard- Rock County Health Dept
Julie Muhle- Beaver Dam Marshfield Medical Center
Marla Noordhof- Beaver Dam Marshfield Medical Center
Abbey Kuehn- Watertown Health Dept.
Sarah Stewart- Watertown Health Dept
Dan Michaels- Public Health Madison and Dane County
Dave Larson- Madison VA Hospital
Joe Meagher- Dodge County Emergency Mgmt
Jodi Moyer- Beloit Health System
Nathan Bubenzer- Meriter UnityPoint Health
Sue Matye- Iowa County Health Dept
Karen Sell- Prairie Ridge Health Columbus
Amy Hollis- Monroe Clinic
Svea Erlandson- WI DHS OPEHC
Brenda Lutz-Hanson- La Crosse County Health Dept
Jeff Ethington- UW Health OPO
Jennifer Behnke- SCWIHERC
SCWIHERC Closed POD Workshop is September 26
Click here for information and registration
June 7, 2019 Meeting
June 7, 2019 Meeting Notes
Meeting slides:
June 7, 2019 Meeting Slides
Hospital Meeting:
Reminders and Updates: The Match Survey is due June 30 for any real events or exercises in which your hospital was a primary player/responder. We use this data to document in kind support because ASPR requires that we match a percentage of our grant funding through in-kind support. If you have your AAR handy, this should take you less than 10 minutes.
Next WISCOM roll call will be June 18, so we can do a radio check for our exercise on June 19. Jennifer will send you a heads up like usual.
We discussed the upcoming SCWIHERC MCI Surge Functional Exercise. Exercise document packets were available at the meeting for attendees. Each packet contains the ExPlan, Controller/Evaluator Handbook, the Master Scenario Events List, the Exercise Evaluation Guides, the Player Briefing, the Communications Plan, a facility sign-in sheet, a Regional Medical Coordination map, and a paper patient packet customized for each facility. The docs will also be emailed out a few days before the exercise, including the communications plan which already needs updates. If you did not attend the meeting in person, Jennifer will mail the packet to you. The controller evaluator briefing will be June 13 at 9:30, and we will have a briefing the morning of the exercise as well.
We discussed the future of the hospital workgroup. Hospital members agreed there is still value to the workgroup. We will include topics like open discussions on hospital-focused lessons learned, regulatory/accreditation compliance, and other topics that come up.
Christal Foreyt discussed the Center for Domestic Preparedness HERT course and talked about opportunities for HAZMAT training and education, and decon team recruitment. We discussed the opportunity for a HAZMAT mutual aid team when a hospital doesn’t have enough internal staff to do a large scale decon operation. We also discussed the need for hospitals to be doing decon drills with their local fire departments. The hospital workgroup will follow up on this topic in the future.
Kyle Schaefer debriefed the SIMCOM 2019 exercise. Our region did a great job responding to WISCOM roll call as part of SIMCOM, we had the highest response rate of the seven regions in the state. This roll call included flipping to the encrypted channel, and we learned a few things about how the encrypted channel works. Kyle and Bill Tyler may follow up with any information learned from the vendors on this.
Membership Meeting
Save the Date: The SCWIHERC Closed POD (point of dispensing) Workshop will be September 26. This will have a presentation on closed POD planning and operations, a panel of representatives from healthcare, a university, and a private business talking about their closed PODS including opportunities for Q&A, and a tabletop exercise with local public health reps to help facilities at all stages of the closed POD planning process.
A reminder that the SCWIHERC MCI Surge Functional Exercise is June 19. There will be many WI Trac alerts that go out that morning, apologies in advance for any alert fatigue. It should be a great opportunity to illustrate SCWIHERC response operations and the regional medical coordination plan, as well as how WI Trac supports information sharing and situational awareness during an incident.
Doodle Polls will be sent out to determine future dates for workgroup meetings. Until each meeting establishes its own agenda and meeting schedule, we will lump similarly themed workgroups to make the most of partner’s travel:
Hospital-surge-evacuation-CMS partners
Special pathogens-public health emergency preparedness (PHEP)-special populations planning.
We discussed and clarified portions of the response plan. ASPR will expect all core disciplines sign off on the plan in the future.
We discussed regional training needs. ASPR places a significant emphasis on training in the new grant, and we have to submit tentative training plans for the year to ASPR by July 31. We also discussed strategies for improving attendance at trainings, as it is not fiscally responsible to offer trainings that are less than 20% full. In the future, SCWIHERC may consider subsidizing travel to trainings to assist partners in attending. A tentative training plan was drafted based on the results of the training needs assessment conducted in late fall/winter 2018, Jennifer will coordinate with other regions to bring these trainings to our region or elsewhere in the state. See meeting slides for details.
Erica Kane from Emergency Medical Services for Children shared a presentation, including EMSC performance measure data for region 5. EMSC also has resources available for pediatric patients, such as comfort kits and pediatric prehospital care guides. Erica can be reached at ekane@chw.org and refer to the slides and their website: https://www.chawisconsin.org/initiatives/emergency-care/emergency-medical-services-for-children/
EMSC Slides
EMSC Presentation June 2019
We talked about measles preparedness for anticipated measles cases in the state. The incident/case response flowchart shared by Public Health Madison Dane County will be distributed by email to the WALHDAB group and public health representatives. We also discussed getting ahead of taking care of our first responder community and others who may be exposed without adequate PPE. All questions should be directed to your local public health officer. The WI DHS Bureau of Communicable Diseases is working on some uniform guidelines and communications resources. The most up to date information from WI DHS can always be found at https://www.dhs.wisconsin.gov/immunization/measles.htm including guidance at the bottom for public health and healthcare organizations.
Cassidy Walsh gave an introduction to the Inventory Management and Tracking System available to health departments for medical countermeasures tracking. More information is at https://www.phe.gov/about/sns/Pages/imats.aspx and in this flyer:
MCM Inventory Management and Tracking System Flyer
We introduced Kim Cox, the new HPP-PHEP program coordinator for WI DHS. She gave some updates from WI DHS including new staff and some new requirements from our new ASPR HPP Cooperative Agreement that starts July 1, 2019. Jennifer also shared some new requirements of note to the membership. See meeting slides for details.
Svea Erlandson, WI DHS State Training and Exercise Coordinator, gave the region an introduction to the Dells-Delton Area Response Exercise Series (DARES) being planned. This is WEM’s capstone exercise for 2020 (2016 was Miles Paratus, 2018 was Dark Sky). With this exercise taking place in our region, and its scenarios involving mass casualty incidents, medical surge, family assistance centers, and mass fatality management. With the unique mix of permanent residents and seasonal visitors to the Dells area, our health partners have a unique opportunity to take advantage of multiple training and exercise opportunities through this series. Contact Jennifer to see the slides shared on DARES. Svea can be reached at charlotte.erlandson@dhs.wisconsin.gov
Meeting Attendance:
Jeff Kindrai- Grant County PH
Sam LaMuro- Fort Healthcare
Gail Scott- Jefferson CO PH
Elizabeth Chilsen- Jefferson Co PH
Donna Haugom- Jefferson Co EM
Jim Acker- Watertown Fire
Alison Chouinard- Rock County PH
Asa Rowan- Community Health Systems
Mary Crowley- Juneau Co PH
Mike Lohmeier- SCWIHERC/UW Health
Jeff Ethington- UW Organ and Tissue Donation
Joni Marty- Green Co PH
Tanna McKeon- Green Co EM
Jane Gervais- Adams Co EM
Nathan Bubenzer- Meriter
Erica Kane- EMSC/CHAW
Libby Halma- EMSC/CHAW
Marla Noordhof- Beaver Dam Community Hospital
Doug Voegeli- PH Madison Dane Co
Sharon Warden- Mile Bluff Medical Center
Christal Foreyt- Gunderson Boscobel Hospital and Clinics
Sharon Foley- Divine Savior Healthcare
Angie Cohen- Grant Regional Health Center
Amy Hollis- Monroe Clinic
Jill Lenz- Columbia Co PH
Tracy Buchman- Stoughton Hospital
Tina Strandlie- Stoughton Hospital
Dave Larson- Madison VA
Cassidy Walsh- Sauk Co PH
Joe Meagher- Dodge Co EM
Jennifer Justus- Mercy Walworth
Mandy McGowan- UnityPoint at Home
Karen Sell- Columbus Community Hospital
Juan Cullum- Mercyhealth Janesville
Stephanie Kuschel- NIPARC
Ron Krause- Mercyhealth
Kyle Schaefer- UW Hospital
Mike Stephens- UW Hospital
Steve Haskell- UW Hospital
Ben EIthun- UW Health AFCH
Barb Kuska- Beloit Health System
Lynda Brereton St. Mary’s Madison
Stephanie Lehmann- SSM Health
Bob Swenarski- St. Mary’s Janesville
Jon Erdmann- Divine Savior Healthcare
Tom Eliison- UW Health
Dan Williams- SCRTAC
Bill Brotzman- Badger Prairie Healthcare Center
Kim Cox- WI DHS OPEHC
Svea Erlandson- WI DHS OPEHC
Online:
Alice Salli- Mendota Mental Health
Allison Davey- Marquette Co PH
Bill Ritzer- Reedsburg Area Medical Center
Brian Allen- Southwest Health
Carmen Luther- Reedsburg Area Medical Center
Elisa Stott- Beaver Dam CH, Beloit MH, Edgerton HHS
Lisa Pickarts- Sauk Prairie Hospital
Sally Blackbourn- Memorial Hospital of Lafayette County
Samantha Marcelain- Gundersen Moundview Hospital
Sharon Rateike- St. Mary’s Janesville
Suzanne Schreiner- Adams Co PH
Sean Marquis- Mercyhealth
SCWIHERC Family Assistance Center Workshop
Click here for resources
SCWIHERC Family Assistance Center Workshop
The SCWIHERC Family Assistance Center Workshop took place on April 4. Thank you for attending!
The After Action Report and Improvement Plan is available here:
FAC Workshop AARIP
Resources mentioned at the workshop:
Reunification:
- The “I Love U guys” Foundation https://iloveuguys.org/index.html#home
- Massachusetts Western Region Homeland Security Advisory Council
http://wrhsac.org/projects-and-initiatives/family-reunification-plan-template/ - SafePlans
https://safeplans.com/family-reunification-resources/ - Readiness and Emergency Management for Schools https://rems.ed.gov/docs/FamilyReunificationSample.pdf
- Post Disaster Reunification of Children – A Nationwide Approach
https://www.fema.gov/media-library/assets/documents/85559 - American Academy of Pediatrics
https://www.aap.org/en-us/Documents/AAP-Reunification-Toolkit.pdf
